Rehabilitation: Medicine’s Forgotten Stepchild
Rehabilitation: Medicine’s Forgotten Stepchild
In medical spaces cross Kenya—and much of East Africa—rehabilitation is treated as an afterthought.
A footnote. A quiet “by the way.”
The conversation is loud around surgery, medication, and mortality. But once a patient survives—once the bleeding stops, the fever breaks, the child is delivered after prolonged labour, or the surgery is declared “successful”—the system quietly steps back and assumes the rest will somehow take care of itself.
It won’t.
This is where rehabilitation comes in: medicine’s forgotten stepchild. It is treated as charity, not as a clinical imperative. Yet rehabilitation is not optional. It is not a luxury for “later.” Rehabilitation is the difference between survival and living.
What we are witnessing in Kenya is not simply a clinical service gap. It is a social and economic failure. It is a failure of health vision—one that is quietly costing the country productivity, dignity, and its future.
Untreated or poorly managed disability limits education, employment, and participation in community life. Families absorb the cost through lost income and unpaid care. The state loses productivity while healthcare costs quietly compound through preventable complications. In the long run, everyone pays.
Professional rehabilitation systems and advocates such as the National Association of Orthopaedic Technologists in Kenya, whose work speaks directly to the gaps outlined here are core to this conversation.

A Growing Crisis We Are Pretending Not to See
The demand for rehabilitation is rising—daily and relentlessly.
- Stroke and cardiovascular disease are increasing sharply.
- Diabetes is no longer a “rich country disease.”
- Our roads are war zones—road traffic accidents maim far more people than they kill.
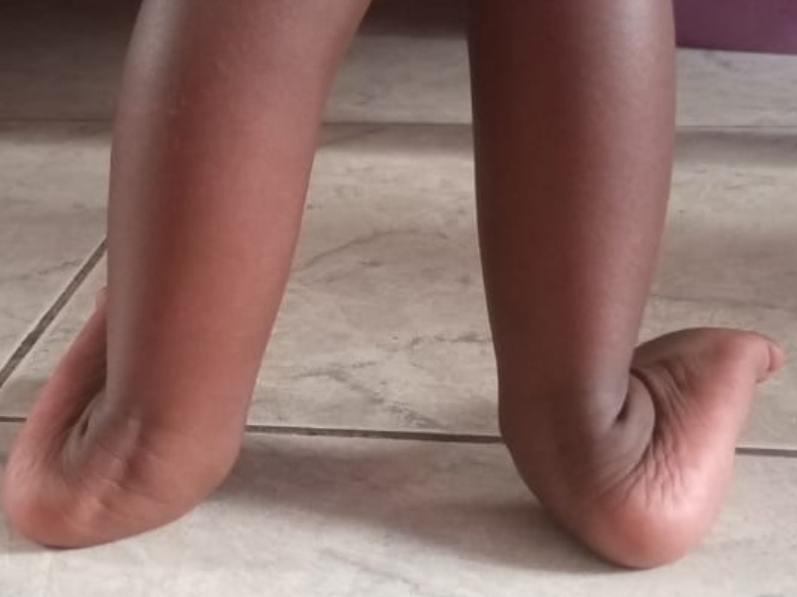
- Congenital conditions such as clubfoot, spina bifida, and cerebral palsy remain under-addressed.
- Violence—domestic, political, and criminal—leaves lifelong disability.
- Cancer survival is improving, with almost no rehabilitation planning.
- Children survive neonatal complications but grow up unsupported.
- Our population is aging, bringing arthritis, frailty, and mobility loss.
The need for rehabilitation is exploding—and we should be alarmed by how little we are doing to prepare.
We build hospitals. We open surgical wings. We buy scanners and post ribbon-cutting photos.
But we rarely ask the harder, more honest question: What happens to people after they survive?
This is not a niche issue. It is a demographic and epidemiological ticking time bomb. We are getting better at saving lives and worse at restoring them. Survival without recovery is neither medically sound nor morally defensible.
Why Rehabilitation Has Always Been Low Priority
Rehabilitation did not suddenly fall into neglect. Its marginalization is structural and historical.
1. A Colonial, Hospital-Centred Model
Kenya inherited a biomedical system designed to fight infectious disease and immediate mortality. TB, malaria, maternal deaths, and later HIV/AIDS dominated policy and funding—and rightly so. But rehabilitation was framed as non-urgent, social rather than medical, optional rather than essential.
That thinking never left. It remains the quiet poison eating away at our health system today.
2. Emergency-Driven Health Financing
Public investment chased what killed fastest. Rehabilitation—which restores function after survival—was excluded from benefit packages, infrastructure planning, and workforce expansion. If you didn’t die, you were assumed to be “fine.”
3. Weak Policy Follow-Through
For years, Kenya lacked a national rehabilitation framework. The Rehabilitative Services and Assistive Technology Strategy (2022–2026) now exists, and the Persons with Disabilities Act (2025) clearly obligates national and county governments to support disability prevention and rehabilitation.
These are important steps.
But without clear financing, accountability, and implementation leadership, rehabilitation remains fragmented, donor-dependent, and politically invisible.
Policy without execution is paperwork—not progress.
4. Politics Follows Noise, Not Need
In Kenya, development follows votes. Roads, schools, hospitals, and strike resolutions attract attention because they generate public pressure. Rehabilitation does not—because its beneficiaries are silent, scattered, and poorly organized.
Until citizens demand rehabilitation services at ward, constituency, and county levels, this neglect will persist.
When Rehabilitation Exists Only as Charity, the System Has Failed
The World Health Organization is clear: rehabilitation is a core component of universal health coverage. It is not a luxury for the few, nor charity for the unlucky. It is essential healthcare.
Yet serious rehabilitation in Kenya is still closely associated with NGOs, missionaries, and foreign charities. While their work helps individuals, it exposes a dangerous truth: when essential healthcare depends on charity, the state has abdicated responsibility.
Between 2022 and 2024, rehabilitation briefly gained momentum. The Ministry of Health, CHAI, and ATscale brought training, equipment, and strategy into the national conversation. Rehabilitation finally had oxygen.
Then U.S. foreign aid was cut. Budgets shrank. The noise died—just like that.
A system that collapses when donor politics change is not a system. It is a gamble. And that gamble is being paid for every day by persons with disabilities, their families, and the general public—who remain viable candidates for disability themselves.
Ignoring rehabilitation does not save money. It simply delays the cost—and multiplies it.

The Medical Hierarchy Problem
A hierarchy exists around healthcare that is hard to ignore.
Trauma is met with swift surgery. Infection is battled with potent drugs. Safe delivery—rightly—is guarded by protocols, specialist teams, budgets, performance indicators, and national dashboards tracking every maternal and neonatal death. These are the visible, celebrated acts of medicine—the stuff of prime-time television, political promises, and hospital billboards.
Rehabilitation, by contrast, is quiet work. It happens after the cameras leave. It is slow, iterative, and deeply human. Progress is measured not in dramatic saves, but in small victories: a first step, a stronger grip, a return to work, independence in daily living.
These outcomes matter profoundly—to patients, families, and the economy—yet they rarely command the same urgency or investment.
Too often, rehabilitation professionals are brought in late—after decisions are made, after opportunities are missed. Something that “a physio can handle.” Something to be sent to “the workshop.”
As a result, rehabilitation sits at the bottom of the healthcare hierarchy—important in theory, optional in practice.
Often, one person is expected to “represent rehab,” as if physiotherapy, prosthetics, occupational therapy, and speech therapy are one thing. They are not.
Rehabilitation is not something you add at the end.
It is a continuum of care that must begin early and be planned deliberately—through services such as those outlined under NAOT Kenya’s professional services.
The Public Is Losing—and Must Push Back
When nurses go on strike, the government moves quickly. Not because it fears nurses alone, but because it fears the uproar of millions of voters who depend on them—from Vanga at the Coast to Wuoth Ogik, Nyatike, Migori County.
Persons with disabilities and their families form a significant voting bloc. They must demand rehabilitation facilities, personnel, and services—from sub-county hospitals upward.
But this fight must not be left to them alone.
If you are not living with disability today, you remain a strong candidate for it—through accidents, disease, strenuous work, or aging. Only death can save you from this.
We must stop celebrating survival alone and start demanding outcomes.
Citizens should ask:
- Where are our rehabilitation units?
- Why are assistive devices paid for out of pocket?
- Why are rehabilitation professionals under-hired?
- Why must patients travel across counties—or countries—for therapy or prosthetics?
- Why is disability treated as social welfare instead of health and development?
Rehabilitation must be embedded in universal health coverage, NCD strategies, road safety policy, maternal and child health, and aging population planning.
Anything less is denial.
Rehab Professionals Must Stop Hiding
Government must act.
The public must demand.
But rehabilitation professionals must also step forward.
Rehabilitation will remain invisible if we hide behind vague labels: medic, daktari, ajuoga, doc, hospital staff. Ambiguity has cost us visibility and influence.
Say what you are.
An Orthopaedic Technologist should say:
I prescribe, design, fabricate, and fit prostheses and orthoses to restore mobility.
Physiotherapists, Occupational Therapists, Speech Therapists, Rehab Nurses—own your scope. Publicly. Consistently.
If we do not define ourselves, others will define us—and badly.
Rehabilitation must be discussed on radio, TV, blogs, newspapers, podcasts, social media, and public barazas. Silence has never built a system. To understand the mandate behind this advocacy, readers can learn more on the NAOT Kenya About Us page.
The Clock Is Ticking
East Africa is urbanizing. Motorization is rising. People are living longer with chronic disease. Survival rates are improving.
This is good news—only if rehabilitation keeps pace.
Without it, progress will mean more disability, more dependency, and more silent suffering.
Rehabilitation is the bridge between medical success and human dignity.
Right now, that bridge is broken.
The question is no longer whether we can afford to invest in rehabilitation.
The real question is simple—and brutal:
Can we afford not to?




Comments